Page Contents
OVERVIEW
This page is dedicated to serving as a comprehensive clinical guide to the topic of breast cancer. Breast cancer can be a difficult subject simply because the disease is spectral and has many different subtypes (each with different outcomes). The structure of this guide is to follow a typical clinical course for disease detection, classification, and progression.
PHYSCIAL EXAM
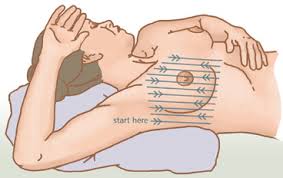
One of the early signs of possible breast cancer can be the detection of unusual masses when physically examining the breast. This can either be from a self examination, from a routine breast/gynecological exam. While many of these findings may be benign, further investigation is required in most cases to characterize the mass in question.
IMAGING
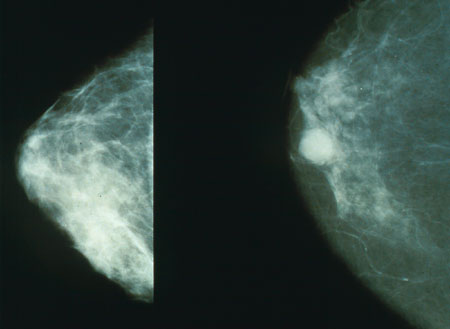
Often times, radiological findings on imaging (that was ordered for a non-breast related issue) can lead to suspicions of breast cancer. Much like general findings on physical examination, the results of such imaging needs to be further characterized to assess for malignancy.
Similarly, when there is already a suspicion of breast cancer in the patient, mammography can be performed to visualize the potential tumor.
BREAST BIOPSY
The decision to perform a FNA vs. a CNB will depend of the patient presentation (FNA is most commonly used for palpable breast lesions). Regardless, the most concrete characterization of suspected breast cancer comes down to historical/cytological analysis.
Hormone receptor analysis: given that there are distinct molecular subtypes of breast cancer, it is important to analyze samples of cells/tissues for the following hormone receptors:
- Estrogen Receptor (ER)
- Progesterone Receptor (PR)
- HER2
Page Updated: 04.28.2016