Page Contents
THE ROLE OF IMAGING: UNDOING MISCONCEPTIONS
Radiologists are often referred to as the “doctor’s doctor”. They may not have direct contact with the patient they are providing care for (although there are exceptions), but they are intimately involved in diagnosis and management decision-making for patients across the continuum of clinical care. Radiologists are routinely called on to help solve puzzles for internists, surgeons, ob/gyns and other physicians. However, there are several misconceptions that doctors-in-training as well as patients may have about the role of radiologic imaging.
- A radiologist’s interpretation of an image is, like other diagnostic tools, a “test” to help diagnose or rule out a condition. However, like other diagnostic tests, it has a sensitivity and specificity that dictates how good it is at picking up abnormalities or excluding abnormalities. This varies from imaging modality to imaging modality, and from person to person. Some modalities are very sensitive at picking up certain pathologies (eg, MRI for tendon tears; or ultrasound for gallbladder stones) but they are not good for other pathologies (eg, MRI is not so good at assessing abnormalities of bone, while ultrasound cannot be used effectively to look at the lungs). Similarly, some radiologists have further sub-specialty training in certain modalities (eg, breast imaging or neuroradiology) that enables them to better identify certain pathologies.
- As I mentioned before, radiologists consider it their job to help solve puzzles or answer questions for other physicians. However, the answer they give can only be as good as the question being asked. For example, if you request a chest x-ray on a patient and the only indication you provide is “?PNA” then you are not giving the radiologist very much context with which to interpret the image and undertake an appropriate differential. Consider the following: what if that patient has a history of tuberculosis? Recent travel? A month-long history of night sweats? Thus, rather than asking for a simplistic rule-out, it is more helpful to provide a very concise and relevant summary of the patient’s history and symptomatology that will allow the image interpreter to think about the right kind of differential.
- Radiologic imaging shows the body at one point in time. It is a very time-limited snapshot into what is going on, and therefore may not reflect a pathology that evolves over time. For example, pneumonia can take some time to appear on an x-ray and also takes some time to resolve. This can be used in our favor to time studies so that we can follow the progression of certain pathologies. However, this also means that sometimes, an image may not capture a problem that is actually happening in the body. This brings me to my next point.
- You must treat the person, and not the image. A patient may have a bowel obstruction that does not show up on a CT scan. But if the patient is lying in the ER with nausea and vomiting, complaining of no passage of stool for some time, and reports a history of abdominal or pelvic surgery, then our instinct should still be strong to treat for a bowel obstruction even if the imaging does not provide conclusive proof.
Imaging is only as good as the technology and the technologist that produces it. Good imaging also relies on the patients’ ability to follow instructions. For example, ultrasound relies heavily on the gestalt of ultrasound technologists, who are not physicians. A barium swallow study requires patients to carefully follow the radiologists’ instructions on when to swallow, when to turn from one side to the next, etc, in order to get a good snapshot in time of the patients’ upper GI function. In such cases, the radiologist has to exercise a lot of judgment in trusting that the pictures they are provided reflect an adequate sample with which to make a full interpretation of the patient.
PRINCIPLES GOVERNING IMAGE PROCESSSING
The practice of radiology requires an exquisite attention to visual detail, an abiding familiarity with human anatomy, and a deep understanding of the macroscopic manifestation of disease. However, practicing sound radiology also requires adherence to principles that help avoid human error and the deceptive shortcuts that our brains are prone to take. These errors can prevent us from analyzing the information in front of us fully. By following certain principles, we can ensure standardized and thorough imaging interpretation. Here are some rules that help govern efficient and effective image processing.
- Before you begin analyzing an image, clearly describe what you are looking at. What type of image is this (eg, ultrasound, MRI, CT), how it has been processed (eg, with or without contrast, with doppler), what orientation (eg, axial, coronal, sagittal) and what body part (eg, abdominal, pelvic, chest). This is important because the things you expect to see or not see can be dramatically different based on the kind of imaging–this helps you to differentiate something normal from something abnormal.
- Always proceed in a uniform order. Radiologists routinely use templates that help them to make sure that they cover all the parts of a particular image series or protocol when they dictate their findings. This ensures completeness and also helps guide the dictation and image analysis. Below is a simplified sample template for a CT scan of the chest with contrast.
- CT CHEST WITH CONTRAST
CLINICAL INDICATION:
FINDINGS:
Chest
Airways/lungs:.
Pleura:
Lymph Nodes:
Great vessels:
Heart/Pericardium:
Esophagus:
Soft Tissues and Bones:
- CT CHEST WITH CONTRAST
- Do not commit an S.O.S.! Satisfaction of search refers to the phenomenon of finding an abnormality on imaging, being satisfied with that finding, and stopping your search for further abnormalities. By using the injunction above to interpret your images completely in a uniform fashion every time, you can avoid this error.
- If you see an abnormality on an image you are analyzing, you should really try to explain why. Imagine the following scenario: you have a 54-year old woman who comes to the ED with shortness of breath. The ED physicians find an elevated d-dimer and are concerned about a pulmonary embolism. Standardized imaging tests, as part of a “PE protocol”, are done and a clot in the pumonary vasculature is found. Do you stop there? No. It is important to consider why this patient should even have a PE. You look further and you find a suspicious lesion in the head of the pancreas. Cancer is known to cause a hypercoagulable state so this may explain why this patient developed a PE. Another example would be a finding of unilateral renal hypoperfusion on an abdominal CT with contrast. Try to figure out why one kidney should be less perfused. Perhaps you may find an aortic dissection!
- Symmetry and homogeneity are your friends. With some exceptions in the body (the heart, the liver, the spleen, etc), the body is pretty symmetric and you should use this to your advantage. If you are looking at an MRI of the brain, for example, and there is increased or decreased signal on one side compared to the other, this should raise a red flag in your own brain. Similarly, if an anatomic structure that is typically uniform suddenly appears heterogeneous on an image, then you should pay attention. For example, simple renal cysts are relatively common and are often pretty uniform in color (ie, homogeneous) in their appearance, whether on ultrasound or CT. This is because they are simply filled with water. However, if a renal lesion suddenly appears to be heterogeneously shaded, then start paying attention. There’s something other than just water in there. It could be a renal cell carcinoma!
IMPORTANCE OF RADIOLOGICAL ANATOM
In medical school, cadaver dissection is a rite of passage. However, it is debatable whether cadaver dissections provide an adequate exposure to clinical anatomy. One thing isn’t debatable however–very few medical students get an introduction to radiologic anatomy as preclinical students (which is why we have a special section dedicated to it on this site). Rarely do we use CT scans in the classroom to learn living anatomy. This means that we don’t get an early enough exposure to anatomy in the form in which it is clinically used! Even surgeons use imaging before they operate to understand a patient’s anatomic structure, and use it to guide their interventions.
Anatomy can be best learned using CT images, as these outline all the structures of the body–bone, soft tissue, vessels, air spaces–beautifully. Radiologic anatomy is helpful to learn the most obvious thing physicians need to know: where things are in the body. It is important to be able to identify where the organs are in all planes. Once you see the body enough times in axial, sagittal, and coronal reconstructions, you start to think in 3D and can visualize in your mind where something would be on the real patient. Interventional radiologists use this process to guide their poking and prodding into blood vessels, abscesses, and tumors.
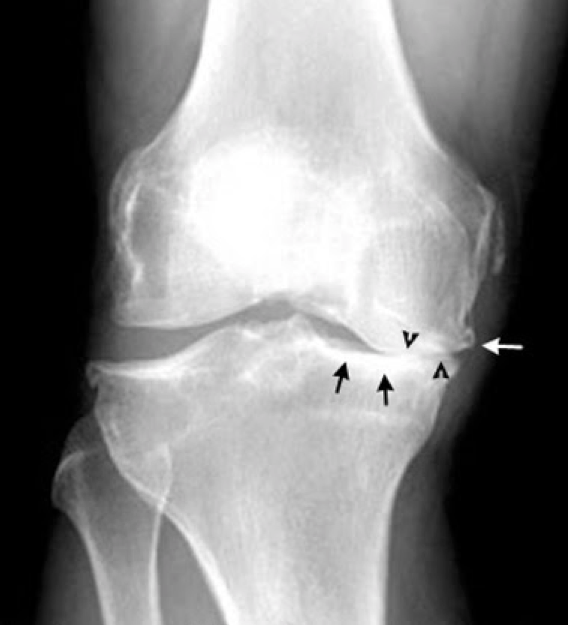
A more sophisticated use of anatomy is to interpret the placement of things in the body using knowledge of normal human embryology and physiology. Where organs are relative to each other is the consequence of early human development. The way in which these organs function is a function of physiology. If you use these principles, you can understand how to interpret imaging findings. For example, the route of metastasis of certain cancers is closely determined by the pathway of lymph vessels that drain from there. Testicular cancer can illustrate this point well. Because the gonads drain to lymphatics that travel along the gonadal vessels to the para-aortic lymph nodes, it is important in a patient with gonadal cancer (ovarian or testicular) to assess for abnormal appearing lymph nodes in the para-aortic space along the kidneys, as this would provide evidence of metastatic disease. A more common example is ascites, which tracks in certain spaces of the peritoneum and in certain extra-peritoneal spaces. Similarly, a good example of how to use physiology to contextualize radiologic anatomic findings is arthritis. Osteoarthritis results from wear and tear on joints, as cartilage between bones breaks down due to overuse. This means that where activity and gravity exert their most potent effect, you see destruction of cartilage and narrowing of joint spaces. This is why when patients have osteoarthritis of the knees, it is often asymmetric, because more weight may be put on one side of the knee joint than the other. Because bone tries to heal in response to this chronic stress, it results in sclerotic bony outgrowths at the margins that are a reaction to bone damage–these are called osteophytes.
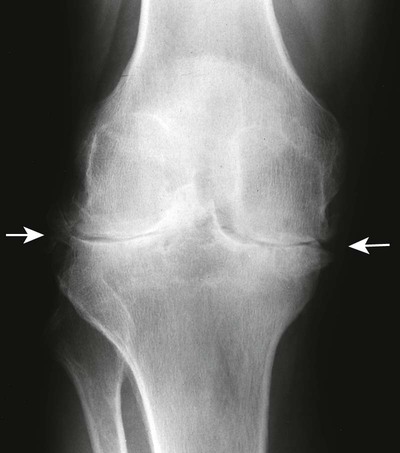
By contrast, rheumatoid arthritis is an autoimmune inflammatory disease of the joints. It attacks the joint lining pretty symmetrically, and thus leads to destruction of bone and cartilage. This means that wherever the synovium (which is inflamed) surrounds the bone, that area will be destroyed and there is no bone outgrowth, while the joint space is more uniformly narrowed because the entire joint is implicated in the inflammatory process.
The last point to remember is that radiologic interpretation is not just about reporting what is being seen on the image in front of you. It also requires an instinct to track and hunt. A familiarity with radiologic anatomy allows you to use reference points to track and find organs that may be hard to find, or to identify organs that are no longer easy to identify because of pathology that has changed their appearance. For example, radiologists often use the gonadal vessels to find the ovaries which can be too small or indistinct to find otherwise. They track the bowel all the way through the abdomen to find the transition point (ie, the blockage point) in someone presenting with symptoms of bowel obstruction. They follow the flow of blood in the vessels to identify clots or bleeds or aneurysms. They also track the density of things to figure out what kind of substance is present in a given space (water versus blood versus pus for example).
ACKNOWLEDGEMENTS
A very special thanks goes to Dr. Zujaja Tauqeer for writing this page!
Page Updated: 02.08.2018