Page Contents
OVERVIEW
This exam is for the screening of an asymptomatic female adult. The various components are organized below in the following fashion:
- Lymph node palpation
- Breast Visualization/Palpation
- Pelvic External Examiantion
- Speculum Examination
- Bimanual Pelvic Examination
- Rectovaginal Bimanual Examination
LYMPH NODE PALPATION
Axillary nodes: make sure to palpate all of the associated lymph nodes that can be found in the axillary area to check for lymphadenopathy. Palpate all 4 folds of the axial (anterior, superior, medial, and lateral on both sides of the body).
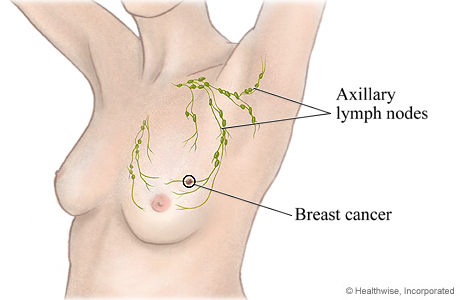
Supraclavicular nodes: as the patient to shrug their shoulders, and palpate hollow areas above the clavicle bilaterally.
Infraclavicular nodes: palpate the area beneath and long the full length of each clavicle (bilaterally)
BREAST VISUALIZATION/PALPATION
Visualization: Using proper draping technique, expose each breast individually and observe for any visual abnormalities.
Palpation: have the patient put their hand behind their head. starting at the sternum, palpate in a vertical strip pattern until reacting the other boundary of the breast tissue. When reading the midline, have the patient twist to an oblique position to better expose the other side of the breast (patient should move hand to forehead).
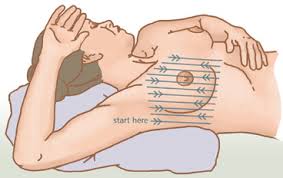
PELVIC EXTERNAL EXAMINATION
MAKE SURE TO WASH HANDS AND WEAR GLOVES!
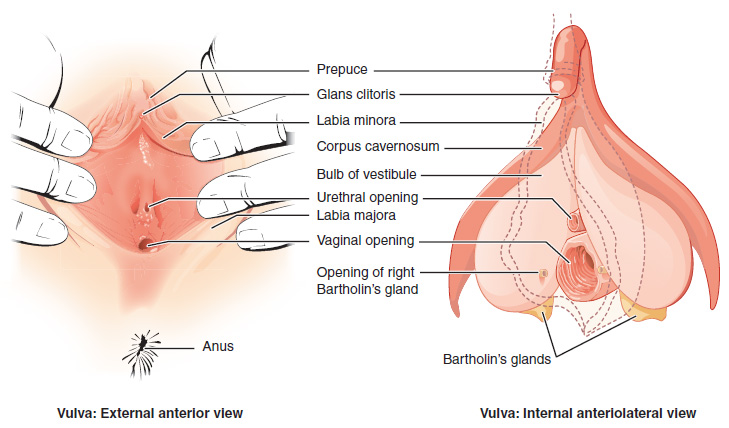
Positioning is a very important aspect of this exam that often is overlooked. After draping have the patient bring their pelvis to the edge of the exam table and position their legs in the stirrups (avoid calling these stirrups usually is a good idea as this can make the patient uncomfortable). As the the patient to “let their knees fall to the sides” so that you can better visualize the genital area. Upon doing all of this, examine the following strucutres:
- Mons pubis (inspect and palpate)
- Labia majora (inspect and palpate)
- Labia minora (inspect and palpate)
- Clitoris (inspect only)
- Prepuce (inspect only)
- Glands (can expose) which include the Skene glands and Bartholin glands.
- Urethral meatus
- Anus
SPECULUM EXAMINATION
Visualization: Before using the speculum make sure that it is an appropriate temperature, and that mechanically it is working. After alerting the patient that the exam is going to begin do the following:
- Spread the labia major using your non-dominant hand.
- Insert the speculum slowly making sure the patient is comfortable.
- Once the speculum is fully inserted then open the blades and try to visualize the cervix.
- After the cervix has been located, lock the bills of the speculum in place.
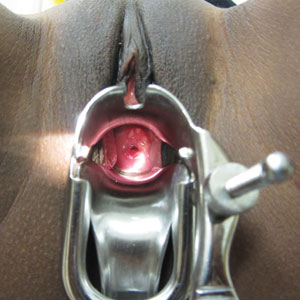
Pap Smear/Routine Culture: after visualizing the cervix, perform the smears/cultures as directed:
- Vaginal: Brushes posterior fornix wall with flat end of Ayers spatula
- Cervical: Inserts narrow end of spatula into cervical os while avoiding contact with vaginal walls and rotates 360 degrees
- Endocervical: Inserts swab slightly moistened with saline or cytobrush solution in endocervix and rotates
Removing speculum: after completing this part of the exam:
- Relax screws while holding blades open
- Withdraw speculum slightly then close blades (to avoid closing the blades on the cervix.
- Rotate speculum while withdrawing to observe anterior/posterior vaginal walls.
- Close speculum completely as it is withdrawn, and withdraw speculum smoothly.
BIMANUAL PELVIC EXAMINATION
As the examiner make sure you are in the standing position, and that you have well lubricated you index and middle finger (of your gloved hand).
- Insert index and middle fingers of gloved hand into vagina (palm up)
- Palpate the cervix
- Palpate body of the uterus between vaginal and abdominal hands.
- Move fingers into the latter affront and attempt to palpate the ovaries.
RECTOVAGINAL BIMANUAL EXAMINATION
Reglove and apply lubricant to the index and middle fingers. Alert the patient that this exam will begin.
- Insert middle finger into the rectum and the index finger into the vagina to full extension.
- Repeat palpation and characterization of the cervix and uterus from the posterior position.
- Palpate posterior wall.
- Palpate rectovaginal septum between fingers while withdrawing hands.
- Withdraw hands smoothly
- Perform guaiac test.
Page Updated: 01.30.2016