Page Contents
- 1 OVERVIEW
- 2 WHAT EXACTLY IS IT?
- 3 WHY IS IT A PROBLEM?
- 4 BEFORE THE WORKUP: PROSPECTIVE GOALS OF HOW TO CLASSIFY PATIENTS
- 5 THE PRIMARY & SECONDARY SURVEYS IN TRAUMA: AN OVERVIEW
- 6 PRIMARY SURVEY: AIRWAY, BREATHING, CIRCULATION (ABCs), DISABILITY, ENVIORMENTAL EXPOSURE
- 7 PRIMARY SURVEY: FAST/eFAST EXAMS:
- 8 PRIMARY SURVEY: X-RAY IMAGING
- 9 POST PRIMARY SURVEY: PATIENT PLACEMENT
- 10 IMPORTANT ACUTE MANAGEMENT OF PELVIC FRACTURE: PLACING A PELVIC BINDER
- 11 SECONDARY SURVEY: HISTORY
- 12 SECONDARY SURVEY: PHYSICAL EXAMINATION
- 13 SECONDARY SURVEY: IMAGING
- 14 SPECIFIC CONSIDERATIONS IN MANAGING PELVIC FRACTURES
OVERVIEW
This page is designed to organize content that is relevant to the topic of pelvic fractures. This type of fracture can often times can be an emergency, and requires a systematic workup.
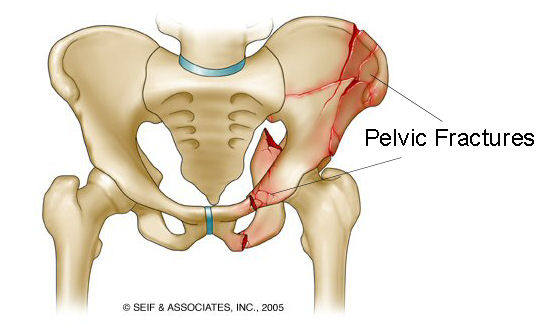
WHAT EXACTLY IS IT?
Before going any farther, let us make sure we clearly define the “medical problem”. A pelvic fracture refers to a pelvic bone that has been broken in some way. Often times motor vehicle accidents are the cause of pelvic fracture, however it can be the result of many different types of trauma.
A pelvic fracture can be suspected/detected early on in a trauma case, felt on the physical exam, seen on X-ray imaging and/or might be initially elected on a CT scan of the pelvis. Regardless of how exactly it is detected/suspected this page will try to provide a central location on how one should approach this medical problem.
WHY IS IT A PROBLEM?
A fractured pelvis is often times associated with very heavy bleeding in the pelvis. Not only can a significant amount of blood be lost (from the actual broken bone itself AND from surrounding structures that are commonly damaged with this fracture), the area of bleeding is hard to control because of its location. Most commonly these pelvic fractures are associated with venous bleeding in the pelvis, however in certain cases arterial bleeding can also occur.
BEFORE THE WORKUP: PROSPECTIVE GOALS OF HOW TO CLASSIFY PATIENTS
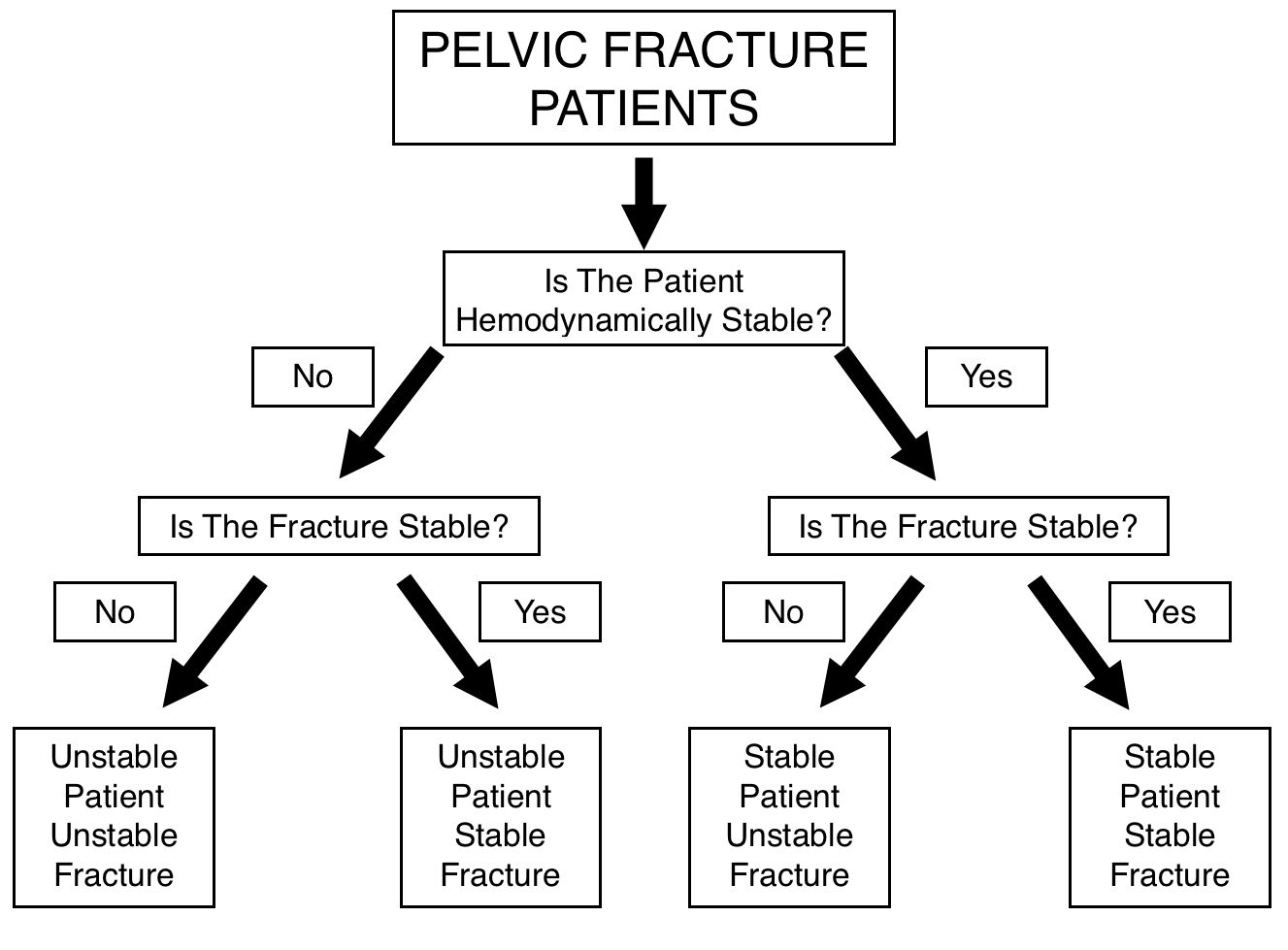
Before diving into how to approach and workup a patient with a suspected/confirmed pelvic fracture it is important to first outline the general goals behind this workup. While there are many questions to answer when working up such a patient, two core questions must be answered
- Is the patient hemodynamically stable?
- Is the pelvic fracture anatomically stable?
While this is of course not the extent of the workup, being able to categorize patients by these two questions will help guide patient management significantly. Each combination of anatomical/hemodynamic stability requires a different approach. One must always remember that the stability of the patient and the anatomic stability of the fracture are not the same thing.
THE PRIMARY & SECONDARY SURVEYS IN TRAUMA: AN OVERVIEW
The primary and secondary surveys in trauma are applied to many different situations (not just for suspected pelvic fractures). That being said, often times pelvic fractures will be detected, and suspected in the context of these surveys (which is why they are listed on the page below).
In brief, these surveys work together to quickly and comprehensively evaluate a patient in a systematic order.
PRIMARY SURVEY: AIRWAY, BREATHING, CIRCULATION (ABCs), DISABILITY, ENVIORMENTAL EXPOSURE
Whether it is evaluation of a new trauma case, or a pelvic fracture that has been confirmed by imaging, evaluating/re-evaluating the ABCs is always important (and often times the first step in the workup). It is during this step that the hemodynamic stability of the patient should be evaluated!
Airway:
Should the C-spine be stabilized? Is the airway obstructed from trauma? Is an advanced airway needed?
Breathing:
Are breath sounds present bilaterally? Are there signs of a tension pneumothorax?
Circulation:
In patients with a suspected/confirmed pelvic fracture a systolic blood pressure < 90 mm Hg is assumed to be caused by hemorrhage until proven otherwise. Patients in this category should begin resuscitation using a massive transfusion protocol.
Disability Assessment:
Evaluate for mental status. Glascow Coma Scale (GCS).
Environmental Exposure (And Everything Else):
Evaluate the entire body for any other type of injury or environmental exposure that could be dangerous to the patient. At this point the pelvis may be palpated/examined to evaluate for any tenderness or signs of a pelvic fracture.
In the case of a pelvic fracture quickly looking for any signs of open fracture in the perineal area, and if time allows, a urethral, vaginal, and rectal exam should be conducted to evaluate for any bleeding in any of these anatomical areas.
PRIMARY SURVEY: FAST/eFAST EXAMS:
The FAST or eFAST exams have become implemented to help quickly evaluate for any signs of bleeding in key areas. It is important to realize that these exams typically will not be able to detect the presence of retroperitoneal or exztraperitoneal bleeding (such as bleeding in the pelvis).
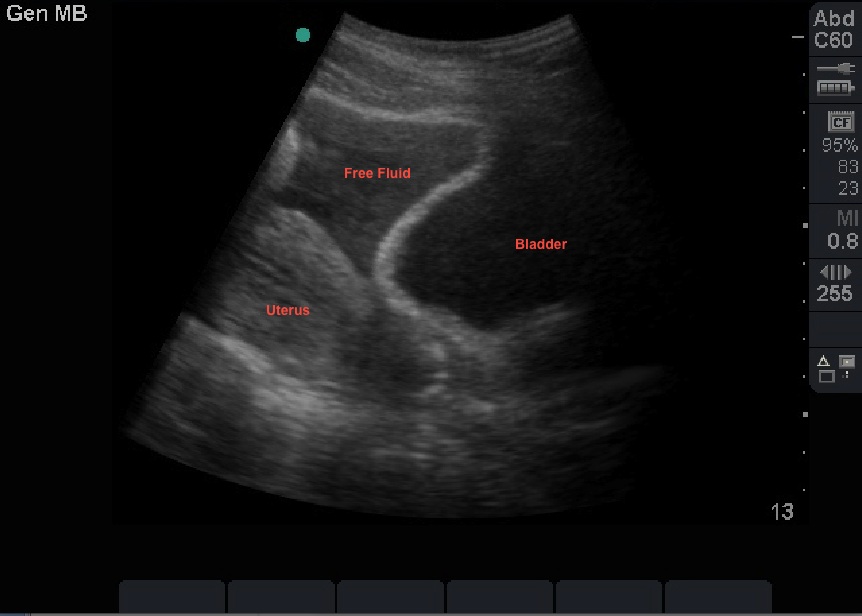
Hemodynamically unstable patients with a positive FAST/eFAST need a trip to the operating room for surgery that will identify and aim to control the source of the bleeding.
PRIMARY SURVEY: X-RAY IMAGING
As an adjunct to the ABCDE’s and FAST/eFAST exams explained above, portable X-rays will also be collected (either after or during components of these exams). Generally speaking a chest X-ray and pelvic X-ray are almost always obtained (especially in a patient that clearly is not hemodynamically stable enough to go to the CT scanner) however in some cases an X-ray of the C-spine may also be obtained.
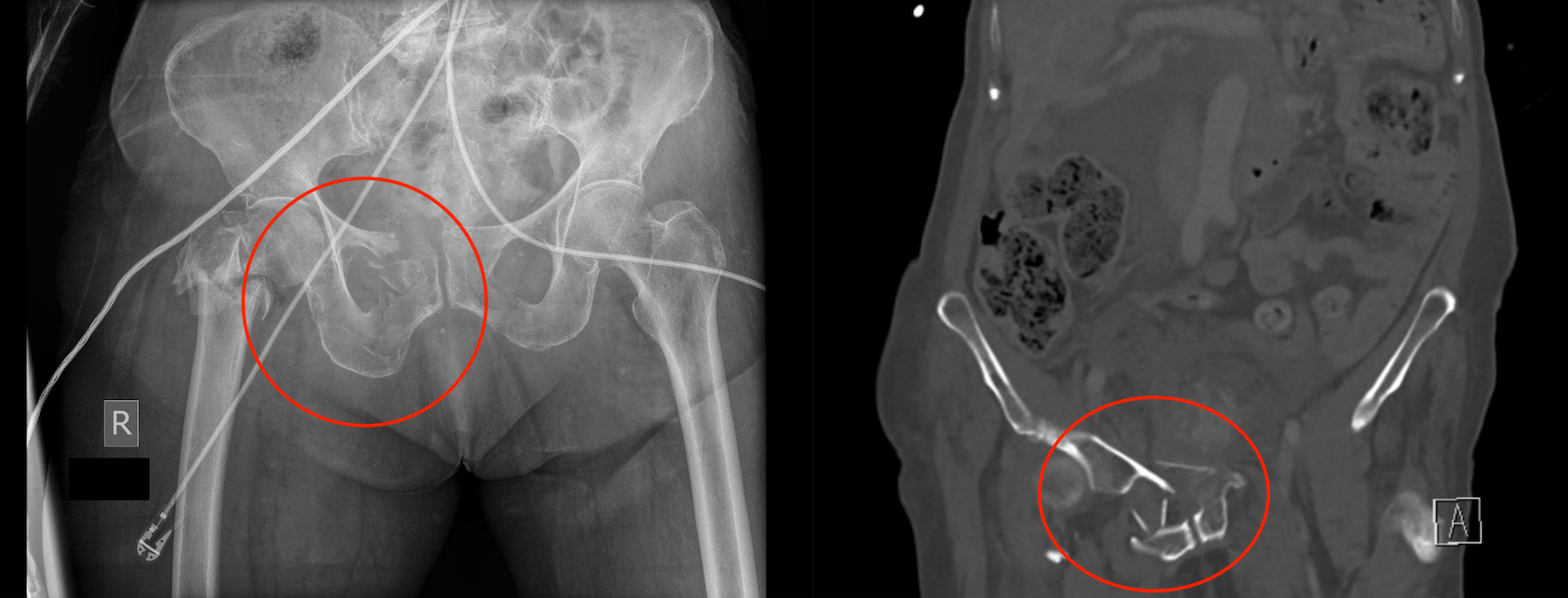
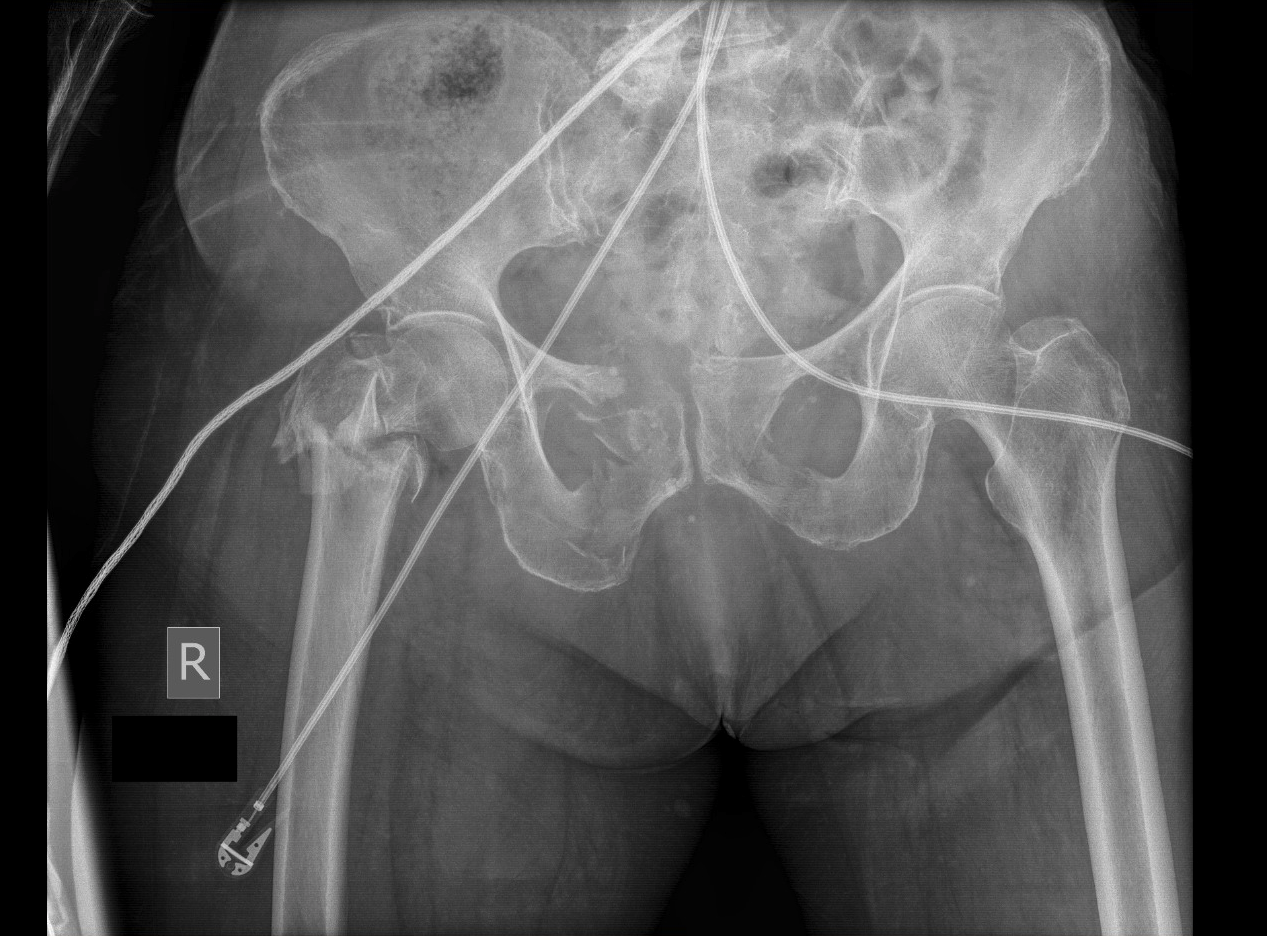
Portable pelvic X-ray:
This X-ray may be the first clear proof that a patient actually has a pelvic fracture. With this in mind, it is important to appreciate that a pelvic X-ray may miss certain pelvic fractures, and that a CT scan of the pelvis is the gold standard for detecting pelvic fractures.
POST PRIMARY SURVEY: PATIENT PLACEMENT
As discussed before, the primary survey will be where the hemodynamic stability of the patient is first evaluated. It will dictate how extensive the workup of the patient will be before a procedural intervention is necessary. With this in mind, the patient’s placement will depend upon the results of this primary survey.
In the case of a hemodynamically unstable patient who is found to have a pelvic fracture: a pelvic binder should be placed (more on this below) and the patient should be quickly taken to a hybrid OR where both open and interventional radiology procedures can be conducted. Trauma, interventional radiology, and orthopedic teams will work together to control the bleeding and stabilize this patient. More detailed considerations on this can be found here. Keep in mind that while the patient is waiting for their procedure to begin some components of the secondary survey (such as key physical exam maneuvers) may be conducted.
In the case of a hemodynamically stable patient: a more extensive workup/secondary survey can be conducted because things are less urgent. The patient may likely still need a procedure to manage their fracture, however more data can be collected without putting the patient’s life in unnecessary danger.
IMPORTANT ACUTE MANAGEMENT OF PELVIC FRACTURE: PLACING A PELVIC BINDER
In most cases, placing a pelvic binder can provide significant benefit, and there rarely will be a contraindication to its placement. Pelvic binders can help stabilize the fracture anatomically AND can help control bleeding in the pelvis (by applying pressure and tamponading bleeding vessels by decreasing the potential space in the pelvis). In this way the judicious application of a pelvic binder can stabilize the patient both hemodynamically and anatomically. This page here will discuss further how to properly place this binder.
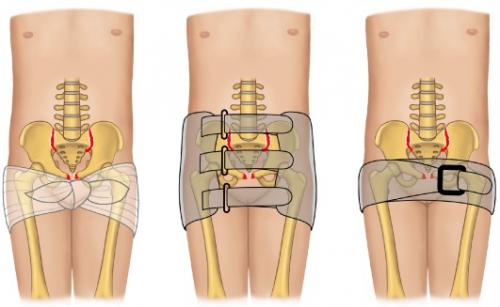
The issue with placing a pelvic binder early on is that it can impede certain components of the physical exam, and can alter the anatomy of the fracture on imaging. It is for this reason that when possible the placement of a pelvic binder is delayed until the physical exam evaluation for damage to the vagina/uterus/urethra/bladder is quickly completed (more on that below). With this in mind, especially in a hemodynamically unstable patient, the binder may be placed before some of these exam components are completed.
Ideally before the pelvic binder is placed the urethra, vagina, and rectum will be examined properly (explained more below in the secondary survey): this can be done very quickly right before the binder is placed.
Once the binder is placed it is important to limit any reason that it will need to be taken off UNTILL the patient has been taken to the OR/IR suite for treatment.
SECONDARY SURVEY: HISTORY
Patient with trauma and pelvic pain should be assumed to have a pelvic fracture. Other components of a history may be necessary to the workup of a patient with recent trauma, however it is important to realize that this is sufficient to reach the threshold of a suspected pelvic fracture.
*Realistically at this point in the secondary survey one should already have imaging that either shows the presence of a pelvic fracture or excludes it.
SECONDARY SURVEY: PHYSICAL EXAMINATION
It is important to appreciate that some of this physical exam may have been performed during the primary survey in the E/”Everything Else” category:
In thinking about evaluating only for a pelvic fracture the physical exam is not necessarily the most extensive. Any tenderness to palpation along the region of the pelvis (in the right trauma context) should be concerning for a pelvic fracture.
In addition, evaluating for any signs of an open fracture. Rocking the pelvis is no longer conducted because it can cause more damage to the area.
Realistically at this point during the secondary survey a pelvic fracture should have already been detected on imaging. Because of this, the physical exam will become less about confirming the radiological diagnosis, and more about evaluating other common injured structures. Here are specific things to focus on WHICH IDEALLY SHOULD BE CONDUCTED BEFORE A PELVIC BINDER IS PUT ON THE PATINET. The findings of this physical exam will directly change patient management and are important.
Signs of open fracture externally (such as in the perineum):
This will have hopefully be conducted during the primary survey, but it is important to make sure that the pelvic fracture does not communicate with areas such as the perineum, as this would make it an open fracture (which is managed differently, with more concern for infection).
Signs of urethral or bladder injury:
This requires a multistep approach to ensure that a foley catheter is not inserted into a damaged urethra:
- Look for blood in the urethral meatus: if it is present DO NOT INSERT A FOLEY. A retrograde urethrogram will be required to evaluate for damage to the urethra.
- If no blood in meatus, insert foley catheter into the bladder: at this point the urine should be evaluated for the presence of blood. If blood is present it strongly suggests damage to the bladder.
Signs of damage to the rectum:
A digital rectal exam should be performed and the presence of blood in the rectum should be assessed. The presence of blood on the rectal exam is highly suggestive of rectal injury in the setting of the pelvic fracture.
Vaginal injury:
Patients with a known pelvic fracture require a pelvic exam (with a speculum if possible) to evaluate for a fracture that extends into the vaginal canal. Such a fracture is classified as being open, and will require altered management because of the higher risk for infection.
SECONDARY SURVEY: IMAGING
Generally at this point an X-ray of the chest and pelvis will have been obtained in the secondary survey, however it is important to appreciate that a CT scan is the gold standard for diagnosing a pelvic fracture. It is for this reason that patients who are hemodynamically stable often will receive a CT scan as part of their workup. It is important to remember that imaging findings do not change the hemodynamic stability of the patient. A more severe/complicated fracture does not mean the patient is in more danger and vice versa independent of their stability.
CT-Scan:
CT is the gold standard for diagnosing a pelvic fracture. It may not always be practical because a patient may be unstable, however it will provide much more useful information regarding the pelvic fracture, and is much more sensitive for detecting a pelvic fracture. A CTA can also be conducted to evaluate for any active areas of bleeding in the abdomen or pelvis.
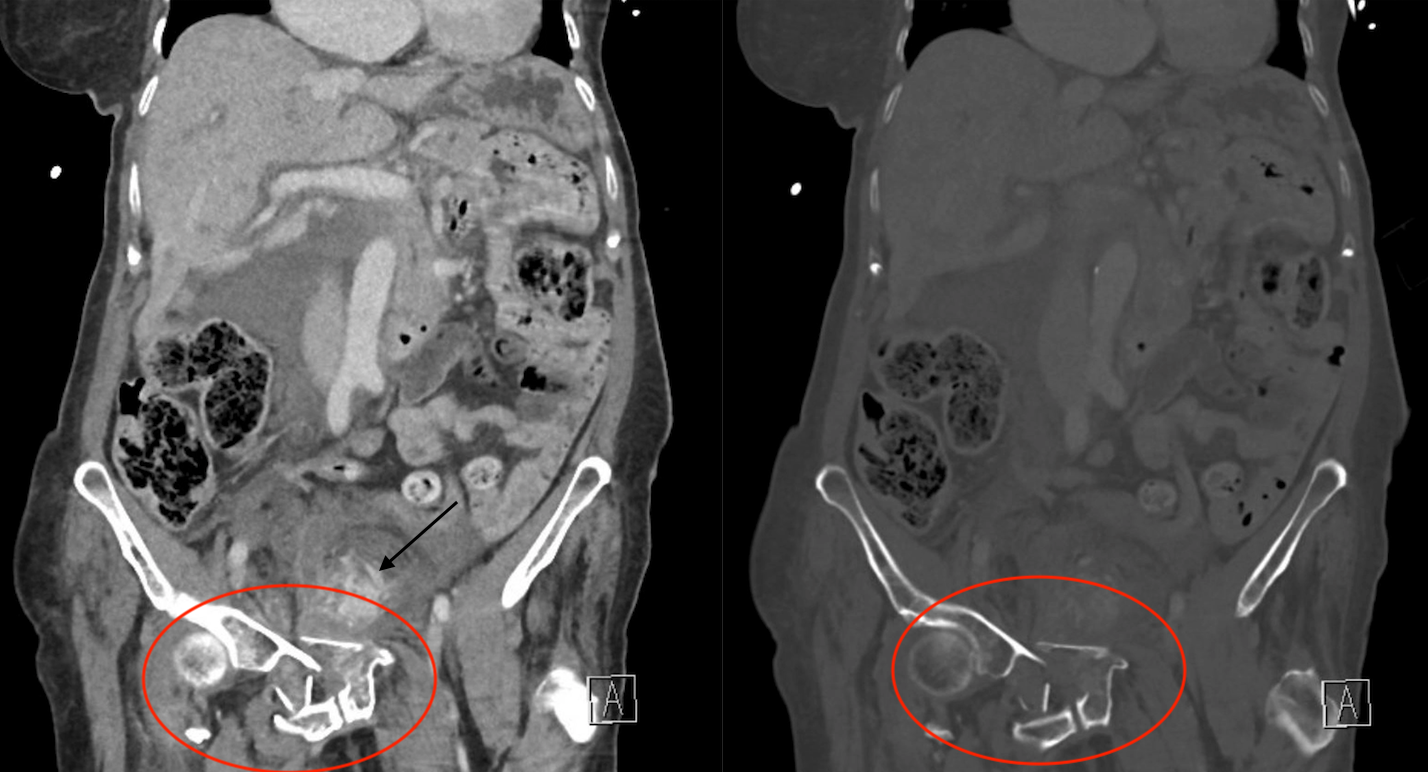
SPECIFIC CONSIDERATIONS IN MANAGING PELVIC FRACTURES
While the above gives a good overview about how to workup/manage a patient with a pelvic fracture, there are more specific considerations that need to be kept in mind that are elaborated upon on the pages below:
- Proper placement of pelvic binders in patients with pelvic fractures
- Procedural management of bleeding for pelvic fractures
- Anatomical stabilization of pelvic fractures
Page Updated: 02.28.2018